Volunteers are the heart of Rally's mission!

Rally Kid Lucy battled Glioblastoma for five months: December 4, 2019-May 13, 2020
WRITTEN BY RALLY MOM EMILY
Lucy was born on November 13, 2015 in Roswell, GA at North Fulton Hospital. I had a normal pregnancy and a textbook delivery. Lucy was the fourth and final beautiful baby girl to complete our family. She was a perfectly healthy child with no sign of illness, until a few weeks after her 4th birthday in Fall 2019.

Lucy with her older sisters: Abby (8), Hope (6) and Hannah (8)
Lucy’s symptoms first presented as a low-grade fever and a stiff neck. Her first visit to the ER was December 1, 2019 and she was diagnosed with a strained neck, called torticollis. After a few sleepless nights and periods of neck and arm spasms, we ended up back in the ER.
My husband, Jonathan, and I explained our neurological concerns and insisted that the doctor watch her walk across the room—something she could barely do. She was off-balance and her muscles were weak.
We ended up discharged with a muscle relaxer for Lucy’s neck muscles. The medication relaxed her enough and allowed her to sleep well for the first time in several nights.
During those 48 hours and two ER trips, I googled torticollis multiple times and the presentation and diagnosis seemed to line up. However, the very next morning, Lucy’s body was mush. She had no motor function in her legs or arms. Was this the medication? After a call and a quick visit to our pediatrician, we knew something was terribly wrong and immediately rushed back to the ER for the third time.
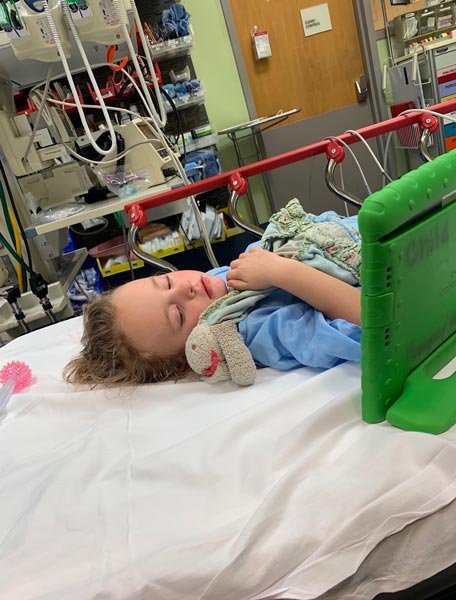
Lucy in the ER
With the new onset of paralysis symptoms, in addition to loss of bladder control, Lucy was sent straight to the trauma room. The doctor walked in within seconds. He was incredibly smart, calm, and reassuring as he asked questions and went down his mental checklist. Based on the low-grade fever and stiff neck, I was certain that it must be some kind of uncommon virus causing this paralysis.
Looking back, I know he knew differently.
Lucy’s bloodwork had been perfect at the other two ER visits, and it was again at this one.
The first thing the doctor wanted was an MRI, but it was almost 7:00 pm. He was able to get approval for the team to start her two-hour MRI immediately. The MRI team all stayed after hours. They didn’t want to sedate Lucy because her condition was so severe, but she would need to lay completely still for two or more hours in a scary and loud machine.
I was able to walk her back and stay in the MRI room with her, rubbing her foot and comforting her anytime she cried. The room was freezing cold and loud, even with the earplugs. They played Mary Poppins on the tiny TV in the MRI machine. Lucy miraculously fell asleep during the scan.
I’ll never forget the conversations that I had in that cold, loud room with God—just me, my youngest daughter strapped down in a big spaceship-looking machine, and God.
My husband and I were reunited and escorted back to the trauma room. The ER doctor met us at the door, sat us down, and then told us the most gut-wrenching, disorienting, life-altering news of our lives.
“The scans show a massive, and likely very aggressive, tumor wrapped in and around her spinal cord. A neurosurgeon is reviewing the slides now and will be in shortly. Lucy will most likely need surgery first thing in the morning.”
I didn’t see that news coming.
I didn’t know anything about MRIs, brain tumors, or the pediatric cancer world. That was all about to change.
Our baby girl had just turned four. I couldn’t understand how such a young and healthy child could have this monster tumor wreaking havoc in her little body.
Our cancer journey began that night, and so did the questions. How long had this been growing? What caused it? How could we have three other perfectly healthy daughters? They all ate the same things, had the same environmental factors and similar genetics. Why was this happening to Lucy? The questions went on and on.
Surgery was scheduled for the next morning—just five days since our first visit to the ER. The surgery lasted eight long hours and required two neurosurgeons, along with a neuromonitoring team of physicians, to give Lucy the best chance of not being paralyzed. After eight grueling hours, they were able to remove 50% of the tumor.
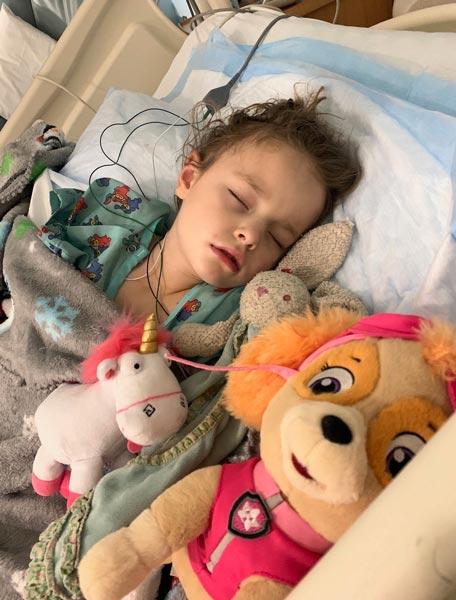
Lucy after her eight-hour surgery
The initial surgical pathology reports came back that most of the tumor was mostly benign cells but also confirmed a glioma or glial tumor. We took a deep breath. We would have to wait on additional pathology reports to determine a “grade”, but initially the tumor didn’t appear to have any of the classic markers indicating it was a high-grade glioma.
Lucy recovered in the Pediatric ICU and was then moved to inpatient rehabilitation to begin the slow and painful recovery of her damaged spinal cord. Over the next five weeks, we would go from celebrating tiny toe wiggles to pedaling the rehab bike. She made great progress. We were so proud of her.

Lucy’s first trip out of the PICU alongside her parents
On Christmas morning, Jonathan, myself, Lucy’s three older sisters, her Grammy, Nani, and Papaw celebrated together on the rehab floor. While Lucy was opening her presents, we noticed a delay in Lucy’s hand movement. We continued to see declining movement for two more days. We shared our concerns with our neurosurgeon, and he ordered a follow-up MRI.
Two days after Christmas, just three weeks post-surgery where 50% of the tumor had been removed, the scan revealed the devastating news that Lucy’s spinal cord tumor had completely grown back to its original pre-surgery size.
Even though the pathology details that were slowly coming back from the lab continued to suggest low-grade malignancy, we all knew with this rapid growth that this glioma tumor was highly aggressive.
We discussed risks and benefits of chemotherapy versus radiation. It was all gut-wrenching with no promising protocol. There was no way to know the long-term effects of these treatment options to her little four-year-old body. Each “what’s the long-term risk” question we asked the doctor was answered with “if she makes it that long.”
Our prayer changed that day and we asked God for quality days over quantity. Jonathan and I decided to trust God with the number of days we would have Lucy and focus on the quality of the days we had left. That was not an easy decision, but it was one we have never regretted.
We decided to fight as aggressively as possible with six weeks of proton radiation. Lucy began the following Monday, December 30, and finished on February 12, 2020.

Lucy with her parents and sisters prior to proton radiation therapy
The post-radiation MRI on March 3, 2020 showed that Lucy’s spinal cord tumor had completely disappeared. We were so excited and thankful.
The very next week, COVID-19 hit and life shut down. We had three weeks straight of precious quality family time with Lucy and her sisters that we will be forever grateful for.

Lucy enjoying a “COVID sleepover” with her mom and sisters
However, on March 30, a short three and a half weeks after finishing proton radiation, Lucy had a grand mal seizure. She ended up being intubated and put in an induced coma. A final MRI scan revealed metastasis all through Lucy’s central nervous system: new cancer lesions down her lower spine, lesions on her brain stem, and an additional tumor in the right frontal lobe of her brain, crossing the mid-section.
We had our diagnosis: Glioblastoma Multiform of the Central Nervous System. Stage 4. No options left.
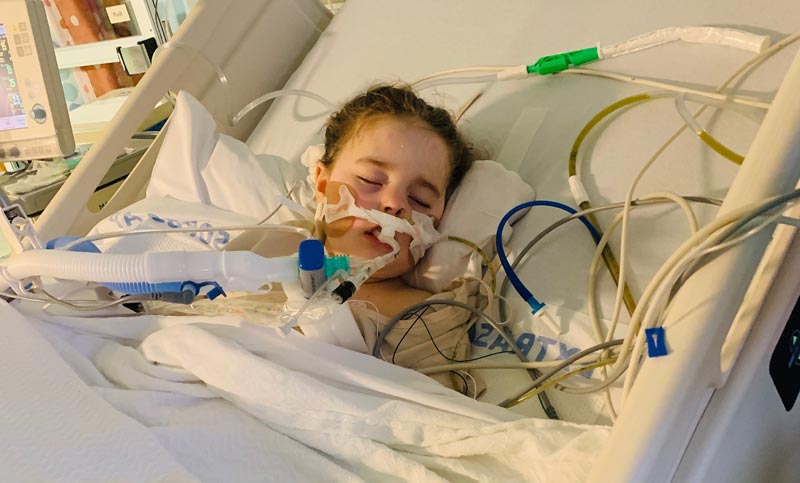
Lucy in the hospital post-seizure
We were able to bring Lucy home on hospice where she spent her final weeks in the comfort of her Mommy and Daddy’s bed, surrounded by family and friends and of course, her three big sisters who love her dearly.
On May 13, 2020, Jonathan was beside me as I held Lucy in my arms. Our parents were there along with our angel hospice nurse and we had the heartbreaking honor of escorting Lucy into heaven. Our precious Lucy’s five-month battle with the deadliest brain cancer, glioblastoma, was over.

Lucy at home with her loving family
GBM Awareness is so desperately needed. During Lucy’s journey, the tumor grew quicker than we or Lucy’s medical team could get information. Multiple teams of Brain & Spinal Cord Tumor experts were stumped by the pathology—the tumor tissue didn’t match the known characteristics of glioblastoma. You see, glioblastoma in children is not the same as glioblastoma in adults. Pediatric GBM tumors have different biology and different research is desperately needed.
We made the very best decisions for Lucy’s GBM based on the information that we had, but we had to make extremely risky treatment decisions with very little information. Children with glioblastomas need better treatment options. Children with GBM need a cure. Parents should never hear the words, “We are sorry. There are no treatment options left.”

In loving memory of Rally Kid Lucy (11/13/15 – 5/13/20)
We know Lucy’s life had a purpose. We think part of that purpose is to raise awareness and funds for pediatric glioblastoma focused research. We asked for an autopsy and that Lucy’s tumors be saved so they could be studied and hopefully provide answers and solutions. We are proud to be a part of the Rally family who will never forget our precious Lucy and who funds the most promising pediatric glioblastoma research through a dual peer-review process.
Before Lucy was diagnosed, we were not aware of GBM. You may not have been aware until Lucy’s diagnosis or until now. But now that you are, please share Lucy’s story and please give to Rally to support cutting-edge pediatric glioblastoma research in honor of Lucy and all kids who have to fight this nasty, deadly brain tumor. Together we can make a difference.
So honored to know and love the Settle family. Their family is a beacon of light in a dark world! Lucy was a spunky, precious, paw patrol loving little light that we had the joy to know.
Kids deserve better, parents need more information when they are in this fight.
BEAUTIFUL BABY We love and miss you XoXo
So sorry that this rapidly developing tumor took Lucy’s life.
I’m so very sorry for the loss of precious Lucy. My heart breaks for you. I have 3 daughters, 3 granddaughters and 2 grandsons. I could not fathom having something like this happening to one of them. I will keep your family in my prayers. May God bless you and ease your pain.
Thank you for sharing our precious granddaughter’s story. May her Light continue to shine and bring awareness to the desperate need for more research and a cure for this devastating disease.